This article is intended for educational purposes only. Consult with your doctor first – always.
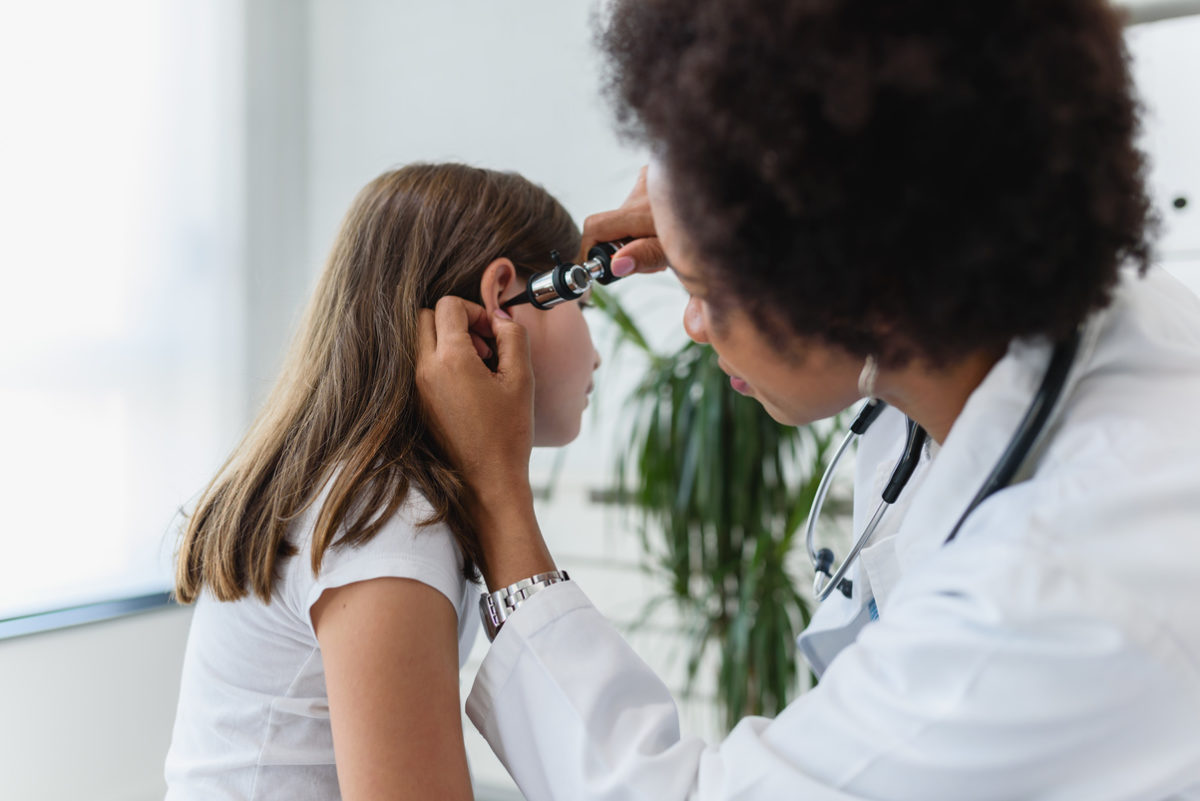
Mr Paul Montgomery – Consultant Ear, Nose & Throat Surgeon at 150 Harley Street talks about Ear canal infections, Acute Otitis Externa.
Ear canal infections occur when either a bacteria or fungus infects the skin of the ear canal. This causes severe pain in the ear with hearing loss, buzzing, itching and a discharge. The ear looks normal, but the ear canal is very tender to touch and often there is a foul discharge. Predisposing factors for otitis externa are swimming, trauma such as removal of wax and diabetes.
Treatment is as follows:
The ear canal debris should be cleaned out by an Ear Specialist to improve the penetration of the anti-bacterial or anti-fungal drops. The debris is sent for testing to determine whether it is either a bacterial or fungal infection.
The most common bacteria to cause this condition are pseudomonas aeruginosa staphylococcus aureus and staphylococcus epidermidis.
The most common bacteria to cause this condition are aspergillus and candida.
In a patient whose ear canal is so narrowed by the infection that the ear drops cannot get in to work then a small wick (called a Pope wick) is inserted into the ear canal. This wick expands using the eardrops and this allows further drops to get in to the ear.
If it is bacterial infection then antibacterial drops such as gentamicin + hydrocortisone (2 drops three times a day for 5 to 7 days) is used.
If it is fungal infection, then antifungal drops such as clotrimazole (2 drops three times a day for 14 days) is used.
It is important not to put in aminoglycosides based ear drops if there is a perforated ear drum as they can harm the inner ear.
Any patient who is diabetic and has otitis externa must be seen immediately by an Ear Specialist as there is a dangerous variant of otitis externa, called malignant otitis externa, which is more likely in the diabetic patient.